A tibial fracture is a painful injury that can seriously affect your quality of life if it isn’t taken care of properly. If you don’t remember what a tibia is, it’s the inner long bone that’s between your knee and ankle that runs parallel to the fibula. It’s also called the shin bone. It’s critical for standing upright and walking because it supports most of your weight. It’s also essential for your knees and ankles to work properly.
Did you know that the tibia is the most commonly fractured long bone in the body? In Canada alone, there are about 11,000 tibial fractures per year.[i]
But how do tibias get broken? Can a tibia fracture with no warning? Is it something that happens over time?
Causes
A tibia can be fractured suddenly by sports accidents, falls, traffic accidents, osteoporosis, and type 2 diabetes, or over time by repetitive movements. Treatment depends on the type of fracture and the damage to the surrounding soft tissue.
In all cases, treatment must be provided by a medical professional; a broken shin bone is a serious injury and should never be treated at home. If you suspect you’ve fractured your tibia, contact a medical professional, and get your shin looked at immediately.
Next, we’ll look at the signs and symptoms of a fractured tibia.
Signs and symptoms
If you’ve got a tibial fracture, you might have localized pain and swelling if you’ve got a hairline fracture. If the break is more severe, you won’t be able to stand on your injured leg, and you might have bruising, deformation, or even bone protruding through the skin. It will be painful and you must seek professional medical attention.
Most fractures will heal, but in some cases, even with the best medical attention, the broken bone will not produce new bone tissue and the broken sections will not fuse together. This is called non-union and can cause a great deal of pain and inconvenience for the patient.[ii] But don’t worry; there is treatment available to heal non-union fractures when they occur.
But are there different kinds of fractures? And what exactly is non-union, and what causes it?
Fractures and Non-Union
There are several types of tibial fractures and they can occur anywhere along the shin bone. These include:
Hairline or stress fractures: These are little, thin cracks in the bone caused by repetitive stress.
Non-displaced or stable fractures: The bone is intact but cracked. The fractured parts line up correctly in their normal position while healing.
Displaced fractures: The crack is so severe that the bone’s alignment is affected. Surgery is required to realign the bone.
Comminuted fractures: The bone is broken into more than two pieces.
Spiral fracture: The bone presents a spiral-shaped fracture, caused by a twisting movement.
Fractures can also be transverse (horizontal), oblique (at an angle), proximal (top of the bone), distal (bottom of the bone), or along the shaft. Fractures are called “open” if they break the skin.
When a fracture heals properly, the bone creates new tissue and the broken parts bond together, just as strong as before the injury happened.
However, delayed union or even non-union can occur. Delayed union means the bones take much longer to heal, while non-union means the fractures don’t heal at all. In both of these cases, the patient can suffer months or even years. Pain and even disability can result from non-union.
But what are the causes of tibial non-union? Why don’t some bones heal properly or at all?
Causes of Tibial Non-Union
The rate of tibial non-union in Canada may be as high as 10%. There are several reasons why tibial non-union might occur, but the main culprits that cause a bone to remain damaged are smoking, soft tissue damage, age, and inadequate fixation and immobilization at the time of treatment. Other factors that play a role in delayed union include fracture type, fracture location and severity, NSAIDs (nonsteroidal anti-inflammatory drugs such as ibuprofen, naproxen or diclofenac), and other medications.
Using tobacco products hurts more than just one’s lungs; along with cancer, smoking can affect the body’s healing processes by slowing it down. Quitting smoking, or never starting in the first place can reduce the risk of non-union.
Soft tissue damage also affects how bones heal after a fracture. The tissue surrounding the bone may have also suffered trauma, and in some cases, the soft tissue itself caused the fracture by pulling on the bones to the point that they break. Soft tissue and soft tissue damage can’t be ignored and must be treated along with the fracture.
Generally speaking, age also influences how broken bones heal. When you’re older, your body’s natural healing processes slow down, and that can increase your risk of non-union if you fracture your tibia. In fact, even though we say that “life begins at 40”, our bones are considered mature by that age, and will not heal as quickly if injured. Advanced age is anything over 60 when it comes to fractures, and is a risk factor for healing.
Finally, if a break isn’t immobilized properly at the start of treatment, the bone will not heal. Poor immobilization can also be caused by patient behavior after hospitalization. For example, if you take off your cast too soon against your doctor’s wishes “because it’s driving you nuts”, you might endanger your recovery.
How Tibial Fractures Heal
Non-surgical treatment
Tibial fractures can be treated with or without surgery, depending on how bad the fracture is. If there is no displacement, you might have a splint placed on your lower leg. The splint allows enough flexibility for swelling in a safe manner while keeping movement down to a minimum.
However, a cast may be put in place instead of a splint to further immobilize the bone. The cast would be removed after several weeks, followed by the use of a removable brace to provide support in the healing process.
On the other hand, displaced fractures, spiral fractures, and comminuted fractures require surgery to realign and immobilize the bones.
Surgical treatment
Intramedullary nailing is the most common surgical method of treating displaced fractures in adults. A metal rod is inserted in the canal of the tibia, passed through the fracture, and is then held in place at the ends of the bone by intramedullary nails. This method is not suitable for children or teenagers as the rods can stunt their growth.
Plates and screws are used when several fragments must be held together. The fragments are put back into their original places, and then plates and screws are attached to the bones’ outer surfaces.
External fixation is used when the other two methods are inadequate. In this case, metal pins or screws are attached below and above the fracture site of the bone. These pins and screws are then attached to a frame outside of the skin. This permits the complete immobilization of the bone, and adjustments can be made externally to optimize healing. This type of surgical intervention is used in children, teenagers, and those whose fractures have pierced the skin. When you require surgery for a tibial fracture, your doctor will also prescribe you painkillers as well as rehabilitation exercises. Your recovery will take up to six months. And, as mentioned earlier, non-union might occur, further complicating things. Luckily, it can be treated.
Low-Intensity Pulsed Ultrasound
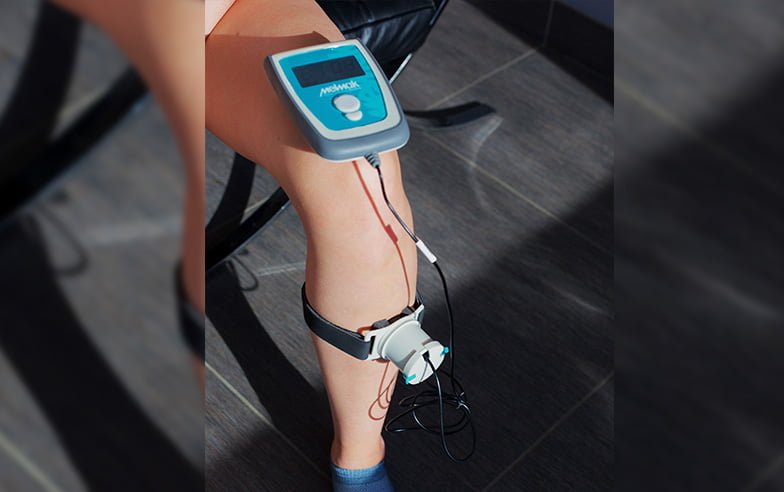
Low-Intensity Pulsed Ultrasound (LIPUS) is a non-invasive, non-surgical technique that uses low intensity pulsed mechanical waves to accelerate healing in fractured bones. The waves produced by a Melmak™-type device stimulate an anti-inflammatory reaction and induce regenerative effects on bone and other tissues in the body. Simply put, it makes your bones grow more bone tissue so the break heals over.
Sometimes doctors will prescribe LIPUS treatment for fresh fractures because it makes bones heal faster. But LIPUS appears to work best when it’s applied to non-union fractures: studies show that they healed by 86%. Treatment with a Melmak™-type device typically lasts about a month, and consists of daily 20-minute sessions- however, the number of sessions may vary depending on the injury. While a LIPUS device may be expensive to purchase, they are available to rent at some clinics. This can help shorten your recovery time and keep your medical expenses low.
Conclusion
A fractured tibia, whether stable or displaced, is no laughing matter. This type of injury must be looked after by a medical professional, and in most cases, follow-up appointments and rehabilitation exercises are required to ensure proper healing.
Smoking, age, osteoporosis, soft tissue damage, inadequate fixation, NSAIDS, other medications, fracture type, fracture severity and location will all affect your recovery and may delay healing. Non-union might even occur, even with the best medical attention, but it can be treated. If you want to recover from your injury, you must follow your doctor’s orders and if you smoke, you might want to quit.
To accelerate healing and prevent non-union, your doctor might also prescribe LIPUS treatment, which is painless, safe, non-invasive, and nothing to be afraid about. Overall, your medical professionals will do everything necessary to get you back on your feet.
[i]Court-Brown C and Caesar B. Epidemiology of adult fractures: A review. Injury. 2006;37:691-697.
[ii]Patel M. Tibial Non-unions. Emedicinemedscapecom. 2015. Available at: http://emedicine.medscape.com/article/1252306-overview#a0199. Accessed April 15, 2015. 4. Wiss D and Stetson W. Tibial Nonunion: Treatment Alternatives. J Am Acad Orthop Surg. 1996;4:249-257




